Tonsillectomy: A ‘Minor’ Procedure With Major Long-Term Risks
Most people only know that sometimes doctors remove tonsils to resolve a problem, such as chronic tonsillitis. Rarely are the potential consequences of this procedure described and neither is the essential role the tonsils play.
In This Article
- Tonsils are a part of the lymphatic system that form a ring-like gatekeeper structure in the throat.
- Because of their strategic importance in our immune system, tonsils have both “gatekeeper” and “messenger” roles.
- Tonsillitis is a process of training and maturation of the tonsils.
- Medical treatment of tonsillitis with antibiotics can have limitations and side effects.
- Natural herbs are beneficial in reducing the symptoms of tonsillitis.
- Combining antibiotics with natural herbal therapies may have a synergistic effect.
- There are a few ways to protect the tonsils.
- Tonsillectomy is often a treatment for severe tonsillitis with enlarged tonsils.
- A 2018 JAMA study of almost 1.2 million children reported that removing the adenoid or tonsils in childhood was associated with a significantly increased relative risk of later respiratory, allergic, and infectious diseases. Increases in long-term absolute disease risks were considerably larger than improvements in the disorders these surgeries aimed to treat.
- A Taiwan national cohort study showed that patients with a history of tonsillectomy had a risk of deep neck infection 1.71 times greater than others.
- A Canadian study suggests a strong association between a history of adenotonsillectomy and the development of retropharyngeal or parapharyngeal abscesses.
- Cumulative evidence of long-term associated risks of infection has proven the irrefutable role of tonsils in our immunity. The mechanism of increased infection relates to various functions of the tonsils in the immune system.
Tonsils as Gatekeepers
The tonsil area is rich in immune cells.
When viruses and bacteria slip through your mouth and nose, the tonsils stand ready, 24 hours a day, guarding the throat—the gate of your body.
Tonsils are lymphatic tissue. They are made up of four parts: the adenoid, the two tubal tonsils, the two palatine tonsils, and the lingual tonsil. Together, these form a robust ring of defense known as Waldeyer’s ring.
The palatine tonsils have about 15 small spaces called crypts, which increase their surface area to increase the capacity to filter external pathogens.
The adenoid, also called the pharyngeal tonsil, is a mass of lymphatic tissue similar to the palatine tonsils that hang from the upper part of the back of the nasal cavity, and along with other parts of the tonsils, can’t be seen. The adenoid tends to shrink after early childhood, and by the teenage years, often disappears almost entirely.
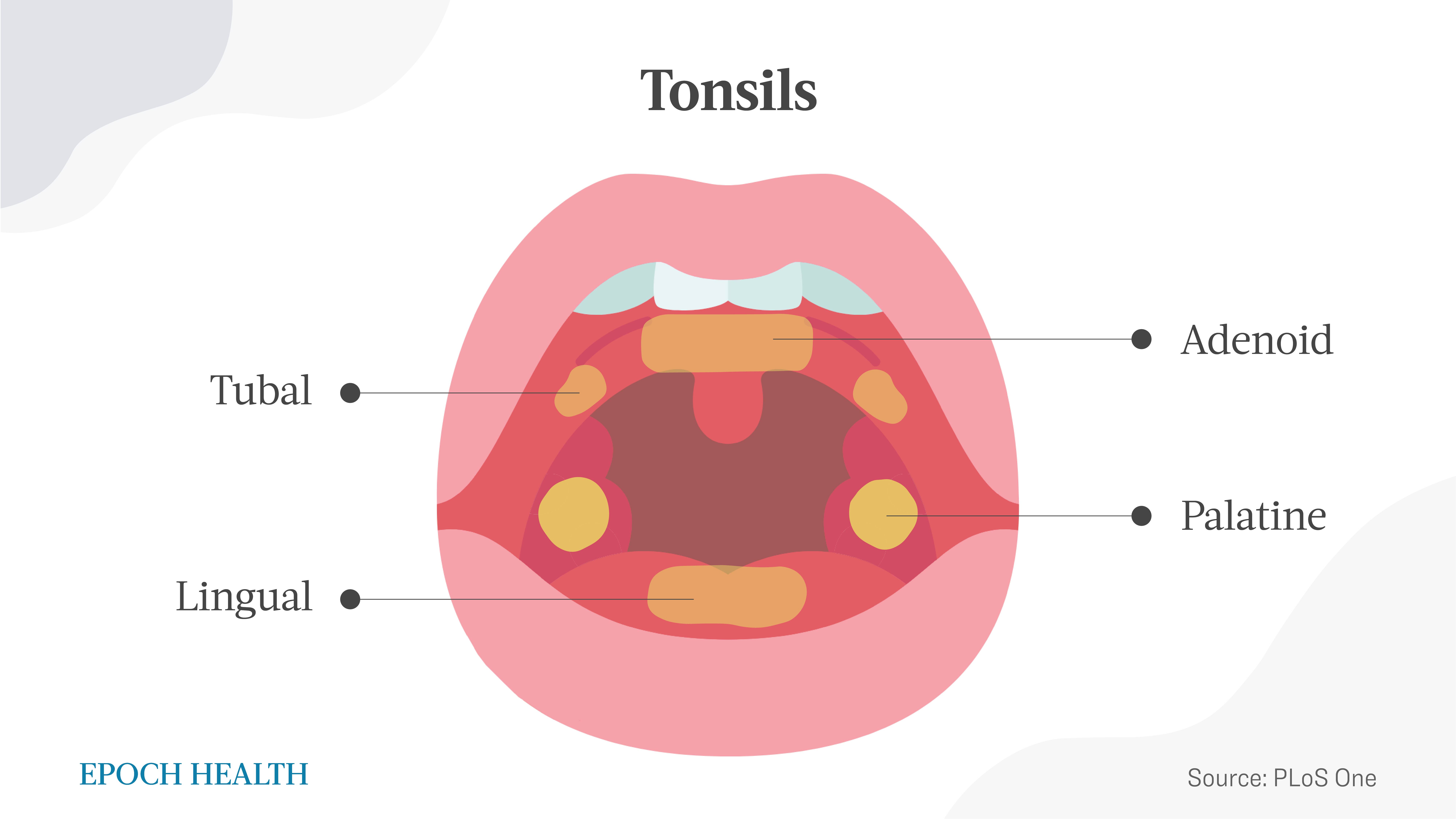
The tonsils’ main job is to trap viruses or germs from the food we eat and the air we inhale. The tonsil area normally gets more blood flow to help fight off common infections.
In short, the tonsils’ role is to protect their territory—you. If these gatekeepers doze off, the enemy, such as a virus, will sneak in. The tonsils use perceptive senses to guard against invaders. They can identify and eliminate the COVID-19 virus and its variants and thousands of other viruses.
Furthermore, according to a study published on March 8 2023 in the journal Nature, tonsil neurons can transmit messenger molecules to the brain to initiate the sickness behaviors during a flu infection that order the body to rest or eat less. This strengthens the tonsils’ role as the body’s gatekeeper and messenger.
We’ve all experienced the power of our tonsils. A common sign of sickness is a sore throat or discomfort in the throat. While we may view it as a minor ailment, we may not be aware that it’s the tonsils warning us of an immune breach and that we should prepare ourselves for battle.
Essential Role in the Immune System
Our tonsils have a layer of epithelial cells that serve as the front-line signal cells detecting and clearing foreign bodies.
These cells are connected by tight junctions, forming a solid barrier against incoming viruses and bacteria. If they sense that invaders may have exceeded their clearance capacity, the epithelial cells will pass the signal to other immunity troops.
There are many specifically designed immune cells specialized in different functions. For example, some cells capture and absorb the antigens produced by viruses and bacteria, some send signals to others, some are good at killing a virus directly, and others can produce antibodies.
Antibodies, a kind of protein, can bind to specific featured fragments of proteins on the surface of a virus. They can neutralize and clear the virus from the body.
Our tonsils house many such cells that can generate various types of antibodies (e.g., IgA, IgD, IgE, IgG, and IgM). Different types of antibodies are like siblings in one big family, generated at various times during an infection or under abnormal conditions, each targeting different cells or tissues.
During fetal growth, the tonsils are among the first regions where many immune cells develop because of their strategic location. They develop early, at about the 14th week of gestation.
Recent research demonstrates that, like the thymus, the tonsils have been shown to express T-cell developmental intermediates that resemble those found in the thymus and bone marrow. That finding could have significant clinical and scientific implications because T-cells are a critical type of white blood cells, immune cells that are the backbone of the adaptive immune response.
Tonsillitis: Process of Learning to Become Stronger
During an exhausting battle against viruses or bacteria, our tonsils may become enlarged, swollen, and red. We will often feel this in the form of discomfort in the throat area. Those are typical signs of tonsillitis. The swelling is caused by a buildup of lymph fluid, viruses, bacteria, and immune cells, and the redness results from increased blood flow to the area.
In 50 to 80 percent of acute tonsillitis cases, viruses such as Epstein-Barr, rhinovirus, respiratory syncytial virus, adenovirus, and coronavirus are the cause. In 5 to 36 percent of cases, the infection is caused by bacteria, with Group A beta-hemolytic streptococci being the most common type in tonsillitis.
Tonsillitis frequently occurs during our younger years, when our tonsils aren’t yet strong enough to combat viruses and bacteria effectively, despite their best efforts. Developing tonsillitis doesn’t necessarily mean our immune system is weak. In fact, it often suggests our immune system is developing and becoming stronger as it learns to fight these invaders.
Recurring tonsillitis during youth indicates dynamics between the tonsils, immune system, and external viruses or germs. Getting tonsillitis doesn’t mean the tonsils aren’t doing their job—it means they are struggling amid the fight. Young tonsils need time to grow stronger. Tonsillitis indicates that the tonsils are overburdened, and it’s a signal for help.
Tonsillitis Treatments and Their Limitations
When the tonsils are exhausted, any method that can help clear viruses or germs, reduce inflammation, or boost immunity will help them recover.
Modern medicine primarily focuses on treating the symptoms of acute tonsillitis by using fluids to rehydrate the body, or drugs, such as pain and fever inhibitors, and corticosteroids to reduce inflammation.
Antibiotics are prescribed if there’s a possibility that bacteria is causing the infection, but it’s often hard to tell just by looking at the symptoms. Moreover, relying on antibiotics can lead to antibiotic-resistant bacteria, which can be harmful. These drugs also damage the microbiome, which plays an essential role in immune function.
Some medications used to treat acute tonsillitis have side effects, such as gastrointestinal bleeding caused by nonsteroidal anti-inflammatory drugs and breath suppression caused by opioids.
Removing the tonsils through surgery is sometimes used to treat recurring acute tonsillitis, but it isn’t usually done during the acute phase of the infection and can have limited long-term benefits.
In addition to antibiotics and other medical interventions, natural herbs can help the tonsils fight back and heal. Combining different forms of therapy may result in a synergistic effect because they work through different mechanisms of action.
Synergistic Ways to Support the Tonsils
Echinacea With Azithromycin
A prospective randomized, controlled study of 300 children with recurrent tonsillitis aimed to measure the effectiveness of prophylactic treatments to prevent recurrence. The study found that the combined use of commercially available echinacea with the antibiotic azithromycin produced better results than azithromycin alone. Azithromycin has been reported to cause adverse events, including lethal heart events, so caution is necessary.
Echinacea comes in various forms, such as supplements, liquids, creams, mouthwashes, and throat sprays. The dosage of echinacea varies depending on the type of product used. It’s important to consult a health care provider to determine the appropriate product type and dosage for a particular condition.
Green Tea
Green tea is a rich source of antioxidants with anti-inflammatory properties. Green tea can also help relieve sore throat symptoms, common of pharyngitis (inflammation of the back of the throat), which often accompanies tonsillitis. Researchers reported in Anesthesiology and Pain Medicine that gargling green tea helps ward off sore throat symptoms in postoperative patients.
Licorice Root, Barberry Root, Thyme, and Oregano
An in vitro (test tube) study investigated hot water infusions of 13 different herbs that can help defend against streptococcal-caused pharyngitis, the most common type of bacterial infection in the throat. Pharyngitis and tonsillitis are closely linked conditions that often share the same cause and treatment. The most effective herbs for pharyngitis according to the study include:
- Licorice root, the fastest and most potent
- Barberry root
- Thyme
- Oregano flowering shoots
Dandelion, Mint, and Skullcap
One systematic review, published in the esteemed Cochrane Database of Systematic Reviews, analyzed 12 randomized controlled trials assessing Chinese herbal medicines for the treatment of sore throat and tonsillitis involving 1,954 participants. The following remedies were found to be more effective than antibiotics in their studies.
Dandelion was more effective than sodium penicillin for acute purulent tonsillitis.
Another treatment mixture was more effective than gentamicin atomized inhalation (nebulization) for acute pharyngitis. It primarily contained the following herbs:
- Mint
- Skullcap
- Wild chrysanthemum
- Honeysuckle
- Houttuynia cordata
Sho-Saiko-To
A recipe called “Sho-saiko-to” has long been recorded in traditional Chinese medicine textbooks to treat pharyngitis or tonsillitis. The recipe is composed of six herbs:
- Bupleurum root
- Scutellaria root
- Ginseng root
- Pinellia tuber
- Glycyrrhiza root
- Ginger rhizome
Japanese researchers tested an adapted recipe, Sho-saiko-to-ka-kikyo-sekko, and reported that it reduced the episodes of chronic tonsillitis for more than two years in a small clinical trial. In some cases, patients even canceled planned tonsillectomies. This recipe added gypsum, Platycodon root, and jujube fruit.
Chinese Herbs
A meta-analysis of 110 randomized controlled trials looked at 12,152 patients with acute tonsilitis. It found that combining Chinese herbal injections with Western medicine resulted in an 89.5 percent improvement in clinical effectiveness, reductions in time to relieve sore throat, red and swollen tonsils, and tonsillar exudate ranging from 76.8 percent to 94.8 percent, and had an incidence of adverse reactions of less than 4.62 percent.
The following key active ingredients were listed:
- Forsythia suspensa
- Vahl
- Lonicera japonica Thunb
- Scutellaria baicalensis Georgi (key ingredient; Baicalin)
- Isatis tinctoria L
- Gardenia jasminoides J.Ellis
Tips to Protect Tonsils
Because tonsils play such a significant role in defense against viruses and germs, maintaining and optimizing their function is advisable.
Most viruses and bacteria are transmitted through the air. Our tonsils are easily overwhelmed when we live in an environment with many pathogens.
- One simple suggestion is to keep our living spaces clean and well-ventilated to reduce the risk of exposure. Additionally, avoiding smoke is crucial, as toxins in smoke are harmful.
- Maintaining proper hydration is also a critical factor in promoting throat health. Adequate air humidity and sufficient water intake can help keep our tonsils healthy.
- Food and drink are other sources of pathogens that can affect throat health, as everything we consume passes through this area. To minimize the risk of exposure, eat organic, nutritious, whole foods. Eating plenty of vegetables and fruits supports the basic functioning of our immune system.
By incorporating more naturally derived remedies into our daily routines, we can also boost our immune system and better support our tonsils to help prevent respiratory illnesses.
Tonsillectomy, or surgical removal of the tonsils, is a common surgical procedure performed more than 500,000 times annually in the United States on children younger than 15 years old. While tonsillectomy may reduce patients’ short-term symptoms, many are unaware of the long-term consequences.
In fact, some diseases are associated with this so-called minor operation.
When Is Tonsillectomy Considered?
Although the tonsils, particularly the adenoid at the upper part, serve as a front line of defense against infection, their role often isn’t adequately recognized.
The tonsils and the adenoid normally shrink with age, being at their largest in children and absent in adults, suggesting that their absence might not affect adult health. However, their activity in early life is essential for normal immune system development and long-term immune function.
When the tonsils are in an intense battle with invading pathogens and don’t get enough support, they may become inflamed and appear larger. As a consequence, these severely enlarged tonsils may cause difficulty swallowing and can obstruct breathing. Since recurrent throat infections and sleep-disordered breathing can significantly affect a child’s health and quality of life, these two factors are common determinants for recommending a tonsillectomy.
In some instances, the adenoid may also be removed through a surgical procedure called adenoidectomy. Generally, physicians recommend the removal of both the tonsils and the adenoid.
According to guidelines from the American Academy of Otolaryngology–Head and Neck Surgery, a tonsillectomy is recommended when a child has had seven or more tonsil infections in a single year, five per year for the preceding two years, or three per year for the preceding three years, in addition to other factors, such as sleep-disordered breathing.
Tonsillectomy: Beneficial or Not?
Will removing the tonsils or adenoid successfully treat illnesses such as recurrent throat infections or obstructive sleep apnea in the long term?
Not necessarily.
The swelling is primarily caused by a buildup of lymph fluid containing viruses, germs, and increased immune cells. Swollen tonsils indicate that too many “soldier” immune cells are injured, suggesting a significant battle between viruses and the immune system. Accordingly, the root cause of tonsillitis is weakened immunity, making it difficult for our body to overcome viruses when more support is needed.
If the tonsils or the adenoid are removed without addressing the underlying cause of the infection—a weakened immunity—relief may be only temporary. The absence of tonsillitis doesn’t mean the viruses or germs are gone, but rather that the guardians are.
In the long term, removing our tonsils leads to the absence of the body’s major first line of defense against viruses and bacteria, leaving us vulnerable to a host of other problems.
Numerous clinical studies have investigated the short- and long-term effects of tonsillectomies on the body. Let’s have a look at the data.
Short-Term Benefits, Long-Term Risks
A 2017 meta-analysis in the journal Pediatrics analyzed illness rates and quality of life for children with recurrent throat infections who had a tonsillectomy versus those instead subjected to “watchful waiting.”
The researchers at Vanderbilt University found that although the benefits of reduced throat infections were evident within a year of tonsillectomy, they didn’t last any longer.
A study examined the effect of tonsillectomy on children with obstructive sleep-disordered breathing. A follow-up one year after the tonsillectomy revealed that these children did have better sleep outcomes than children who didn’t undergo a tonsillectomy, but longer-term outcome measures were lacking.
Despite being viewed as a relatively insignificant surgery, tonsillectomy in children poses a significant risk of complications such as bleeding, respiratory difficulties, burns, nausea, vomiting, pain and, in severe cases, even death.
A Cincinnati Children’s Hospital Medical Center study reviewed 233 claims from the LexisNexis “Jury Verdicts and Settlements” database. The researchers examined claims filed from 1984 through 2010 for “deaths and complications during and following tonsillectomy.”
Of the 233 claims, 96 were deaths, and nearly half (48 percent) were related to surgery. Nonfatal injuries included postoperative bleeding, impaired function, anoxic events, and postoperative opioid toxicity.
Large JAMA Study Revealed Long-Term Risks
A research paper published in JAMA Otolaryngology in 2018 reported the long-term relative risk for 28 diseases after removing tonsils or the adenoid. The study had surprisingly shown that children with their tonsils, adenoid, or both removed before age 9 were at significantly increased risk for a broad range of diseases as they grew older.
The study followed a large cohort of more than 1.18 million Danish children for 10 to 30 years. Of the children analyzed, 17,460 received adenoidectomy, 11,830 underwent tonsillectomy, and 31,377 had both removed; a group of 1,157,684 children composed the control group.
The researchers found that tonsillectomy was associated with a nearly tripled risk of upper respiratory tract diseases, most of which were infections, including rhinitis, pharyngitis, tonsillitis, and laryngitis, which are considered common conditions that everyone experiences during their lifetime.
Furthermore, adenoidectomy was associated with twice the risk of chronic obstructive pulmonary disorder and nearly double the relative risk of upper respiratory tract diseases and conjunctivitis. Additionally, adenotonsillectomy was associated with a 17 percent increased risk of infectious disease.
For 78 percent of the 28 disease groups examined, there were slight but notable rises in relative risk for a variety of diseases.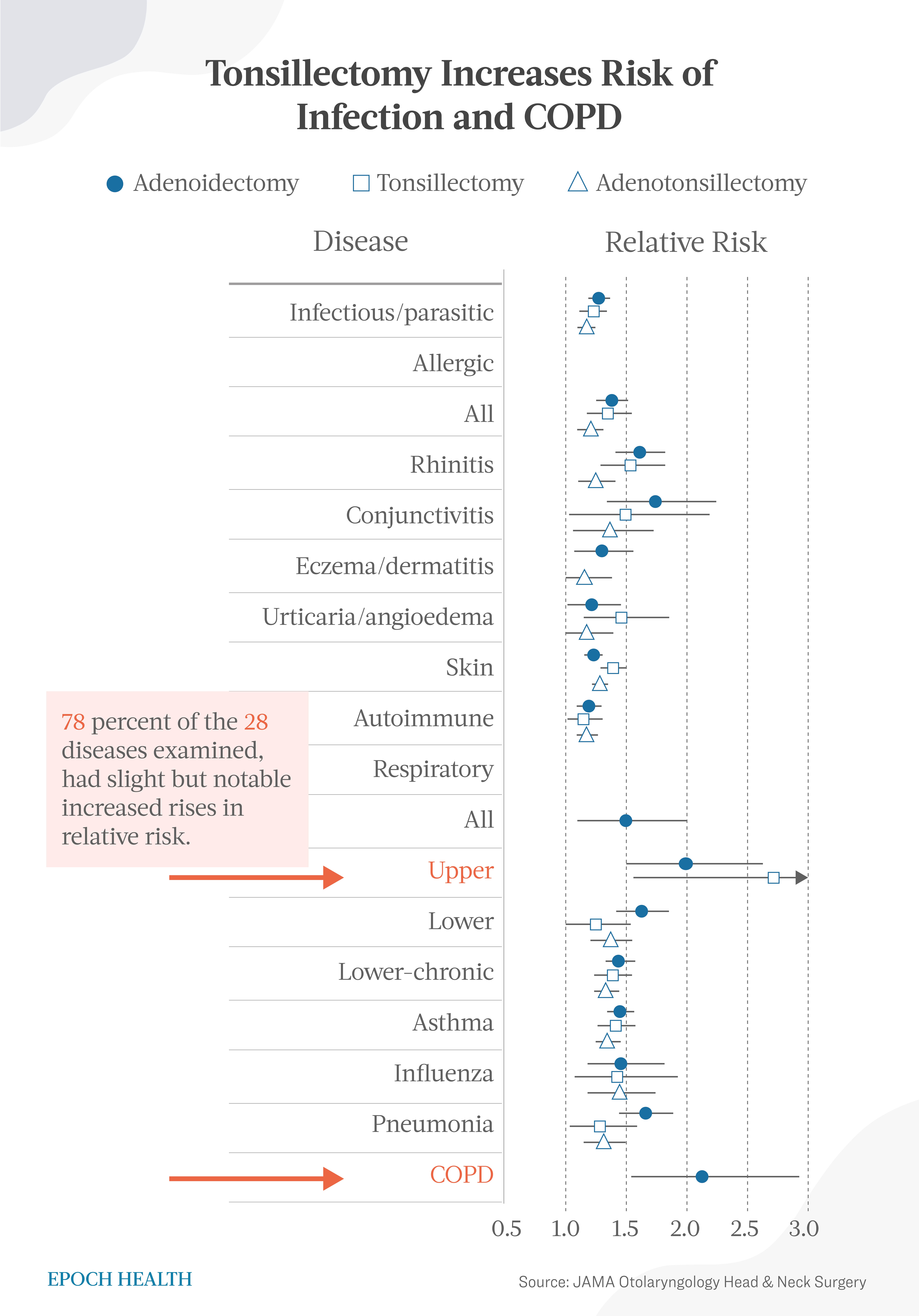
If a data point falls to the right side of the vertical line at 1.0, the surgery indicated by that shape increases the risk of that type of disease. (The Epoch Times)
Those who underwent surgery may also have a higher risk of breathing difficulties, sinusitis, chronic sinusitis, and ear infections.
This highlights the importance of the adenoid and tonsils for normal immune system development and suggests that removal early in life may slightly but significantly disrupt many processes important for health later in life. The authors concluded that it’s important to consider long-term risks when considering tonsillectomy or adenoidectomy.
The JAMA study also found that although surgery to remove tonsils and the adenoid can improve short-term sleep disorders and tonsillitis, long-term risks are similar to not having the surgery.
Increased Risk of Deep Neck Infection
A retrospective, nationwide cohort study using data from the Taiwan National Health Insurance Claims database, which covered more than 98 percent of the population and medical institutions, identified that the risk of deep neck infection is significantly increased among patients who have undergone a tonsillectomy.
A total of 9,915 tonsillectomized patients and 99,150 comparison cohorts between 2001 and 2009 were enrolled in this study. Deep neck infections in the study included abscesses of the throat and neck and cellulitis.
After accounting for confounding factors, those with a history of tonsillectomy had a 1.71-fold higher risk of deep neck infection, according to both statistical models.
Increased Risk of Throat and Neck Abscess: Canadian Study
A Canadian study found that children who had undergone an adenotonsillectomy were more likely to develop a retropharyngeal or parapharyngeal abscess—a buildup of pus in the throat or neck region.
The study examined 180 children with these abscesses and 180 age-matched children without abscesses. Results showed that 13.9 percent of children with an abscess had previously had an adenotonsillectomy, six times more than the 2.2 percent of children in the control group.
The study suggests a strong association between a history of adenotonsillectomy and the development of retropharyngeal or parapharyngeal abscesses.
Mechanism of Increased Risk of Infection
Why is removing the tonsils and the adenoid linked with a greater risk of respiratory diseases and infections?
First, during childhood and early life, the tonsils play a pivotal role in the maturation of the immune system, acting as advanced scouts of bacteria and viruses in food and the air.
Second, an Iran case-control study published in 2020 found that antibody levels after tonsillectomy in 64 children aged 9 to 15 years were significantly lower after four to six years than in the control group.
Additional studies observed a decrease in the serum antibody immunoglobulin A (IgA) level of patients post-tonsillectomy at one to four months, four to six years, and up to 20 years later.
IgA is the major isotype of protective proteins in the surface layer of the respiratory tract and plays a key role in protecting against bacterial, viral, and other infections. Falling IgA levels could contribute to an increased proinflammatory status and an increased risk of infection.
Third, the tonsils—specifically palatine tonsils—express several antimicrobial peptides, including defensins and cathelicidins. They have direct antimicrobial activities protecting the host from microbial invasion and can indirectly modulate adaptive immunity.
Fourth, the tonsils act as a key link between innate and adaptive immunity. Research shows statistically significant decreases in cellular function after tonsillectomy, suggesting tonsillectomy also alters cellular immunity in children.
Removing the tonsils can impair the detection of the virus or germs, decrease mucosal antibody levels, decrease other protective peptides, alter the expression of host defense peptides, alter innate immunity, and increase susceptibility to viral and bacterial infections.
Natural Herbs Help Heal After Tonsillectomy
If you’ve had your tonsils removed or want to give your immune system some support, there are many herbs that can help. These herbs have antioxidant, anti-inflammatory, immuno-modulatory, analgesic, antiviral, antitussive, antimicrobial, bronchodilating, mast cell stabilization, anti-allergic, antihistaminic, and smooth muscle relaxant effects.
A systematic review published in Physics and Chemistry of the Earth identified medicinal plants that can be used to potentially manage respiratory infections. Out of 160 plants:
- 56 alleviated colds, including mint, mango, Shakama plum, larger tinsel flower, lavender, ginger, spearmint, and wild tamarind.
- 53 alleviated pneumonia, including pumpkin, gardenia and cape jasmine, star apple, Christmas berry, and small mahogany.
- 34 alleviated coughs, including mango, parsley, aloe, mint, guava, ginger, and spearmint.
- 29 alleviated chest pain and related conditions, including parsley, cowpea, and larger tinsel flower.
- 25 alleviated asthma, including mango, garlic, parsley, aloe, gardenia, and cape jasmine.
- 22 alleviated tuberculosis and spots in the lungs, including mango, parsley, aloe, and wild tamarind.
- 20 alleviated unspecified respiratory conditions, including Shakama plum and small mahogany.
- 13 alleviated influenza, including guava, ginger, golden everlasting, and wild tamarind.
- 12 alleviated bronchial problems, including wild grape, Shakama plum, and ginger bush.
- Seven alleviated shortness of breath, including Christmas berry and small mahogany.
- Five alleviated sore throat and infections, including star apple and small fig tree.
- One, pepper bark tree, alleviated sinus congestion.
Of the 160 plants studied, 129 exhibited pharmacological properties that aid in treating respiratory conditions. The most common properties were antioxidant, anti-inflammatory, antiviral, and antimicrobial activities, which explains why these medicinal plants have effectively alleviated respiratory illnesses and infections.
References
Baugh, R. F., Archer, S. M., Mitchell, R. B., Rosenfeld, R. M., Amin, R., Burns, J. J., Darrow, D. H., Giordano, T., Litman, R. S., Li, K. K., Mannix, M. E., Schwartz, R. H., Setzen, G., Wald, E. R., Wall, E., Sandberg, G., Patel, M. M., & American Academy of Otolaryngology-Head and Neck Surgery Foundation (2011). Clinical practice guideline: tonsillectomy in children. Otolaryngology—head and neck surgery: official journal of American Academy of Otolaryngology-Head and Neck Surgery, 144(1 Suppl), S1–S30. https://doi.org/10.1177/0194599810389949
Meegalla N, Downs BW. Anatomy, Head and Neck, Palatine Tonsil (Faucial Tonsils) [Updated 2022 Jun 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538296/#
Bin, NR., Prescott, S.L., Horio, N. et al. An airway-to-brain sensory pathway mediates influenza-induced sickness. Nature (2023). https://doi.org/10.1038/s41586-023-05796-0
Drew L. (2023). How the brain senses a flu infection – and orders the body to rest. Nature, 10.1038/d41586-023-00675-0. Advance online publication. https://doi.org/10.1038/d41586-023-00675-0
von Gaudecker, B., & Müller-Hermelink, H. K. (1982). The development of the human tonsilla palatina. Cell and tissue research, 224(3), 579–600. https://doi.org/10.1007/BF00213754
McClory S, Hughes T, Freud AG, Briercheck EL, Martin C, Trimboli AJ, Yu J, Zhang X, Leone G, Nuovo G, Caligiuri MA. Evidence for a stepwise program of extrathymic T cell development within the human tonsil. J Clin Invest. 2012 Apr;122(4):1403-15. doi: 10.1172/JCI46125.
Tai, F. W. D., & McAlindon, M. E. (2021). Non-steroidal anti-inflammatory drugs and the gastrointestinal tract. Clinical medicine (London, England), 21(2), 131–134. https://doi.org/10.7861/clinmed.2021-0039.
Kiyatkin E. A. (2019). Respiratory depression and brain hypoxia induced by opioid drugs: Morphine, oxycodone, heroin, and fentanyl. Neuropharmacology, 151, 219–226. https://doi.org/10.1016/j.neuropharm.2019.02.008.
Abdel-Naby Awad OG. Echinacea can help with Azithromycin in prevention of recurrent tonsillitis in children. Am J Otolaryngol. 2020 Jul-Aug;41(4):102344. doi: 10.1016/j.amjoto.2019.102344.
Huang, Y., Wu, T., Zeng, L., & Li, S. (2012). Chinese medicinal herbs for sore throat. The Cochrane database of systematic reviews, (3), CD004877. https://doi.org/10.1002/14651858.CD004877.pub3
Zaroff JG, Cheetham TC, Palmetto N, et al. Association of Azithromycin Use With Cardiovascular Mortality. JAMA Netw Open. 2020;3(6):e208199. doi:10.1001/jamanetworkopen.2020.8199
Goto, F., Asama, Y., & Ogawa, K. (2010). Sho-saiko-to-ka-kikyo-sekko as an alternative treatment for chronic tonsillitis to avoid surgery. Complementary therapies in clinical practice, 16(4), 216–218. https://doi.org/10.1016/j.ctcp.2010.02.006
Jafari H, Ariaeifar MR, Yazdani Charati J, Soleimani A, Nasiri Formi E. The Effect of Green Tea Gargle Solution on Sore Throat After Coronary Artery Bypass Grafting: A Randomized Clinical Trial. Anesth Pain Med. 2016 May 9;6(3):e32108. doi: 10.5812/aapm.32108.
Wijesundara NM, Rupasinghe HPV. Herbal Tea for the Management of Pharyngitis: Inhibition of Streptococcus pyogenes Growth and Biofilm Formation by Herbal Infusions. Biomedicines. 2019; 7(3):63. https://doi.org/10.3390/biomedicines7030063
El-Anwar, M. W., Elzayat, S., & Fouad, Y. A. (2020). ENT manifestation in COVID-19 patients. Auris, nasus, larynx, 47(4), 559–564. https://doi.org/10.1016/j.anl.2020.06.003
Capriotti, V., Mattioli, F., Guida, F., Marcuzzo, A. V., Lo Manto, A., Martone, A., Molinari, G., Fabbris, C., Menegaldo, A., Calvanese, L., Latini, G., Cingolani, C., Gradoni, P., Boscolo Nata, F., De Sisti, C., Selle, V., Leone, G., Indelicato, P., Pilolli, F., Mevio, N., … Tirelli, G. (2021). COVID-19 in the tonsillectomised population. Acta otorhinolaryngologica Italica : organo ufficiale della Societa italiana di otorinolaringologia e chirurgia cervico-facciale, 41(3), 197–205. https://doi.org/10.14639/0392-100X-N1436
Descamps, G., Verset, L., Trelcat, A., Hopkins, C., Lechien, J. R., Journe, F., & Saussez, S. (2020). ACE2 Protein Landscape in the Head and Neck Region: The Conundrum of SARS-CoV-2 Infection. Biology, 9(8), 235. https://doi.org/10.3390/biology9080235
Qin, L., Zhang, Z., Guo, M., Zhang, Q., Wang, Q., Lu, Z., Zhao, H., Liu, Y., Fu, S., Wang, M., & Gao, X. (2016). Plasma metabolomics combined with lipidomics profiling reveals the potential antipyretic mechanisms of Qingkailing injection in a rat model. Chemico-biological interactions, 254, 24–33. https://doi.org/10.1016/j.cbi.2016.05.022
Gao, X., Guo, M., Peng, L., Zhao, B., Su, J., Liu, H., Zhang, L., Bai, X., & Qiao, Y. (2013). UPLC Q-TOF/MS-Based Metabolic Profiling of Urine Reveals the Novel Antipyretic Mechanisms of Qingkailing Injection in a Rat Model of Yeast-Induced Pyrexia. Evidence-based complementary and alternative medicine : eCAM, 2013, 864747. https://doi.org/10.1155/2013/864747
Shang, W., Wang, X. S., Zou, D. Y., Zhang, Z. N., Liao, X. R., & Yuan, J. (2013). Zhongguo Zhong xi yi jie he za zhi Zhongguo Zhongxiyi jiehe zazhi = Chinese journal of integrated traditional and Western medicine, 33(4), 506–509.
Tang, Y., Wang, Z., Huo, C., Guo, X., Yang, G., Wang, M., Tian, H., Hu, Y., & Dong, H. (2018). Antiviral effects of Shuanghuanglian injection powder against influenza A virus H5N1 in vitro and in vivo. Microbial pathogenesis, 121, 318–324. https://doi.org/10.1016/j.micpath.2018.06.004
Su, H. X., Yao, S., Zhao, W. F., Li, M. J., Liu, J., Shang, W. J., Xie, H., Ke, C. Q., Hu, H. C., Gao, M. N., Yu, K. Q., Liu, H., Shen, J. S., Tang, W., Zhang, L. K., Xiao, G. F., Ni, L., Wang, D. W., Zuo, J. P., Jiang, H. L., … Xu, Y. C. (2020). Anti-SARS-CoV-2 activities in vitro of Shuanghuanglian preparations and bioactive ingredients. Acta pharmacologica Sinica, 41(9), 1167–1177. https://doi.org/10.1038/s41401-020-0483-6
Chen, X., Howard, O. M., Yang, X., Wang, L., Oppenheim, J. J., & Krakauer, T. (2002). Effects of Shuanghuanglian and Qingkailing, two multi-components of traditional Chinese medicinal preparations, on human leukocyte function. Life sciences, 70(24), 2897–2913. https://doi.org/10.1016/s0024-3205(02)01541-2
Windfuhr, J. P., Toepfner, N., Steffen, G., Waldfahrer, F., & Berner, R. (2016). Clinical practice guideline: tonsillitis I. Diagnostics and nonsurgical management. European archives of oto-rhino-laryngology : official journal of the European Federation of Oto-Rhino-Laryngological Societies (EUFOS) : affiliated with the German Society for Oto-Rhino-Laryngology – Head and Neck Surgery, 273(4), 973–987. https://doi.org/10.1007/s00405-015-3872-6
Bird, J. H., Biggs, T. C., & King, E. V. (2014). Controversies in the management of acute tonsillitis: an evidence-based review. Clinical otolaryngology : official journal of ENT-UK ; official journal of Netherlands Society for Oto-Rhino-Laryngology & Cervico-Facial Surgery, 39(6), 368–374. https://doi.org/10.1111/coa.12299
Morad, A., Sathe, N. A., Francis, D. O., McPheeters, M. L., & Chinnadurai, S. (2017). Tonsillectomy Versus Watchful Waiting for Recurrent Throat Infection: A Systematic Review. Pediatrics, 139(2), e20163490. https://doi.org/10.1542/peds.2016-3490
Bohr C, Shermetaro C. Tonsillectomy and Adenoidectomy. [Updated 2022 Aug 19]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK536942/
Baugh, R. F., Archer, S. M., Mitchell, R. B., Rosenfeld, R. M., Amin, R., Burns, J. J., Darrow, D. H., Giordano, T., Litman, R. S., Li, K. K., Mannix, M. E., Schwartz, R. H., Setzen, G., Wald, E. R., Wall, E., Sandberg, G., Patel, M. M., & American Academy of Otolaryngology-Head and Neck Surgery Foundation (2011). Clinical practice guideline: tonsillectomy in children. Otolaryngology–head and neck surgery: official journal of American Academy of Otolaryngology-Head and Neck Surgery, 144(1 Suppl), S1–S30. https://doi.org/10.1177/0194599810389949
Morad, A., Sathe, N. A., Francis, D. O., McPheeters, M. L., & Chinnadurai, S. (2017). Tonsillectomy Versus Watchful Waiting for Recurrent Throat Infection: A Systematic Review. Pediatrics, 139(2), e20163490. https://doi.org/10.1542/peds.2016-3490
Chinnadurai, S., Jordan, A. K., Sathe, N. A., Fonnesbeck, C., McPheeters, M. L., & Francis, D. O. (2017). Tonsillectomy for Obstructive Sleep-Disordered Breathing: A Meta-analysis. Pediatrics, 139(2), e20163491. https://doi.org/10.1542/peds.2016-3491
Subramanyam, R., Varughese, A., Willging, J. P., & Sadhasivam, S. (2013). Future of pediatric tonsillectomy and perioperative outcomes. International journal of pediatric otorhinolaryngology, 77(2), 194–199. https://doi.org/10.1016/j.ijporl.2012.10.016
Byars SG, Stearns SC, Boomsma JJ. Association of Long-Term Risk of Respiratory, Allergic, and Infectious Diseases With Removal of Adenoids and Tonsils in Childhood. JAMA Otolaryngol Head Neck Surg. 2018;144(7):594–603. doi:10.1001/jamaoto.2018.0614
Thomas M, Bomar PA. Upper Respiratory Tract Infection. [Updated 2022 Jun 27]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK532961/
COPD: Symptoms, Diagnosis, and Treatment. Accessed on March 14 2023: https://www.cdc.gov/copd/features/copd-symptoms-diagnosis-treatment.html
COPD Treatment. Accessed on March 14 2023: https://www.nhlbi.nih.gov/health/copd/treatment
Wang, Y. P., Wang, M. C., Lin, H. C., Lee, K. S., & Chou, P. (2015). Tonsillectomy and the risk for deep neck infection-a nationwide cohort study. PloS one, 10(4), e0117535. https://doi.org/10.1371/journal.pone.0117535
Duval, M., & Daniel, S. J. (2008). Retropharyngeal and parapharyngeal abscesses or phlegmons in children. Is there an association with adenotonsillectomy? International journal of pediatric otorhinolaryngology, 72(12), 1765–1769. https://doi.org/10.1016/j.ijporl.2008.07.007
Hanson, M. A., & Gluckman, P. D. (2008). Developmental origins of health and disease: new insights. Basic & clinical pharmacology & toxicology, 102(2), 90–93. https://doi.org/10.1111/j.1742-7843.2007.00186.x
Radman M, Ferdousi A, Khorramdel Azad H, Jalali P. Long-term impacts of tonsillectomy on children’s immune functions. J Family Med Prim Care. 2020 Mar 26;9(3):1483-1487. doi: 10.4103/jfmpc.jfmpc_935_19
Cantani, A., Bellioni, P., Salvinelli, F., & Businco, L. (1986). Serum immunoglobulins and secretory IgA deficiency in tonsillectomies children. Annals of allergy, 57(6), 413–416.
Radman, M., Ferdousi, A., Khorramdelazad, H., & Jalali, P. (2020). Long-term impacts of tonsillectomy on children’s immune functions. Journal of family medicine and primary care, 9(3), 1483–1487. https://doi.org/10.4103/jfmpc.jfmpc_935_19
Andreu-Ballester, J. C., Pérez-Griera, J., Ballester, F., Colomer-Rubio, E., Ortiz-Tarín, I., & Peñarroja Otero, C. (2007). Secretory immunoglobulin A (sIgA) deficiency in serum of patients with GALTectomy (appendectomy and tonsillectomy). Clinical immunology (Orlando, Fla.), 123(3), 289–297. https://doi.org/10.1016/j.clim.2007.02.004
Rodríguez, A., Tjärnlund, A., Ivanji, J., Singh, M., García, I., Williams, A., Marsh, P. D., Troye-Blomberg, M., & Fernández, C. (2005). Role of IgA in the defense against respiratory infections IgA deficient mice exhibited increased susceptibility to intranasal infection with Mycobacterium bovis BCG. Vaccine, 23(20), 2565–2572. https://doi.org/10.1016/j.vaccine.2004.11.032
Rodríguez, A., Rottenberg, M., Tjärnlund, A., & Fernández, C. (2006). Immunoglobulin A and CD8 T-cell mucosal immune defenses protect against intranasal infection with Chlamydia pneumoniae. Scandinavian journal of immunology, 63(3), 177–183. https://doi.org/10.1111/j.1365-3083.2006.01725.x
Choi, K. Y., Chow, L. N., & Mookherjee, N. (2012). Cationic host defense peptides: multifaceted role in immune modulation and inflammation. Journal of Innate Immunity, 4(4), 361–370. https://doi.org/10.1159/000336630
Kościuczuk, E. M., Lisowski, P., Jarczak, J., Strzałkowska, N., Jóźwik, A., Horbańczuk, J., Krzyżewski, J., Zwierzchowski, L., & Bagnicka, E. (2012). Cathelicidins: family of antimicrobial peptides. A review. Molecular biology reports, 39(12), 10957–10970. https://doi.org/10.1007/s11033-012-1997-x
Moreno, P. M., Sanchez, M., Sainz, M., & Gutierrez, F. (1992). Changes in Immunological Response in Tonsillectomized Children. II. Decreased cellular response. Clinical otolaryngology and allied sciences, 17(5), 380–382. https://doi.org/10.1111/j.1365-2273.1992.tb01678.x
Nyagumbo, E., Pote, W., Shopo, B., Nyirenda, T., Chagonda, I., Mapaya, R. J., Maunganidze, F., Mavengere, W. N., Mawere, C., Mutasa, I., Kademeteme, E., Maroyi, A., Taderera, T., & Bhebhe, M. (2022). Medicinal plants used for the management of respiratory diseases in Zimbabwe: Review and perspectives potential management of COVID-19. Physics and chemistry of the earth (2002), 128, 103232. https://doi.org/10.1016/j.pce.2022.103232
Sources




.png)
.jpeg)



Comments